Age Related Macular Degeneration
WHAT IS MACULAR DEGENERATION?
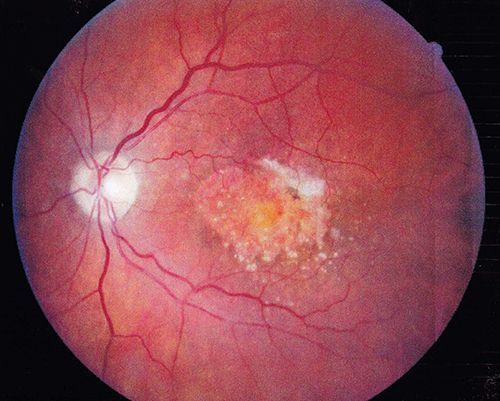
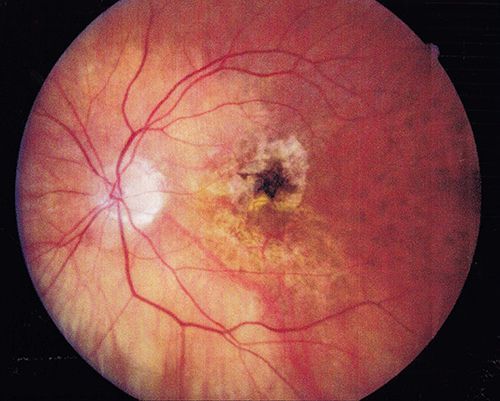
Age Related Macular Degeneration (ARMD) is a retinal condition where the light-sensing cells in the macula malfunction and over time, cease to work. According to the American Academy of Ophthalmology, it is the leading cause of central vision loss (blindness) in the United States today for those over the age of 50.
ARMD is divided into a “dry” or nonexudative form and a “wet” or exudative form. Eighty-five to ninety percent of cases are categorized as “dry” macular degeneration where deposits known as drusen, slowly build up behind the macula, the part of the retina that sees fine details. Dry macular degeneration tends to progress slowly and most patients will maintain reading vision in at least one eye. Ten to fifteen percent of cases involve the growth of abnormal blood vessels under the retina. These cases are called “wet” macular degeneration due to the leakage of blood and fluid into the macula. Wet macular degeneration usually begins as the dry form and is responsible for 90% of severe visual loss in macular degeneration. If allowed to continue without treatment, it can rapidly damage the macula, resulting in missing or blurred vision in the central vision. The peripheral part of the vision almost always remains intact in both wet and dry macular degeneration.
ARE THERE ANY TREATMENTS FOR MACULAR DEGENERATION?
Yes, there are treatments for both the wet and dry forms of macular degeneration.
For many years, laser photocoagulation was the only treatment for the leakage and bleeding associated with wet macular degeneration. Unfortunately it damaged the retina, which in many cases prevented any improvement in vision. Approximately fifteen years ago, laser treatment was mostly replaced with photodynamic therapy, although improvement in vision was still rare.
Since around 2005, newer medications such as Lucentis and Avastin and Eylea have significantly improved the visual results compared with earlier treatments for wet macular degeneration. These medications are injected regularly into the eye and counteract vascular endothelial growth factor (VEGF), which is thought to stimulate the growth of the abnormal blood vessel seen in wet macular degeneration. With this treatment, 90% of patients have stabilization of their vision and 30% can show a significant improvement over one to two years. Unfortunately, the treatment is not a cure, and similar to other conditions such as high blood pressure, continued treatment is usually necessary to maintain maximum benefit. Regular examinations, ancillary testing such as OCT scans and fluorescein angiography, and injection therapy, while challenging for patients and caregivers, are necessary to maintain the best vision and quality of life in patients with wet macular degeneration.
Vitamin therapy can be useful for dry macular degeneration. The Age Related Eye Disease Studies (AREDS) have shown that many patients with dry macular degeneration can benefit from vitamin therapy. AREDS 2 vitamins can reduce the rate of vision threatening complications by over 25% when they are taken regularly over several years. Also, avoiding smoking and maintaining a healthy diet and lifestyle are useful for patients with dry macular degeneration. Eye doctors and retinal specialists can determine whether vitamin therapy is appropriate for you. Regular eye exams can detect changes in the back of the eye due to macular degeneration.
What are the RISK FACTORs for Age related macular degeneration?
Risk factors for macular degeneration include:
- Age
- Smoking
- Family History
- High Blood Pressure
- High Cholesterol
- Poor Diet
- Ethnicity (especially Caucasian)
People with risk factors for macular degeneration should see an eye doctor. Regular follow up appointments, vitamin therapy, and lifestyle optimization may be recommended and are important.
What are the symptoms of macular degeneration?
Patients with macular degeneration may notice problems with their vision. It may be difficult to see fine print or details. Pieces may be missing in the vision. Distortion may occur, where straight lines appear bent or crooked. Any of these symptoms, or worsening of these symptoms, should prompt patients with macular degeneration, or at risk for macular degeneration, to seek care from an eye doctor.
Sometimes, macular degeneration can progress without the patient knowing or noticing problems.
Advanced Retina Associates offices are located in
Orange City and
Port Orange
Advanced Retina Associates, Dr Lieb.
Site Design by Infinity Medical Marketing.