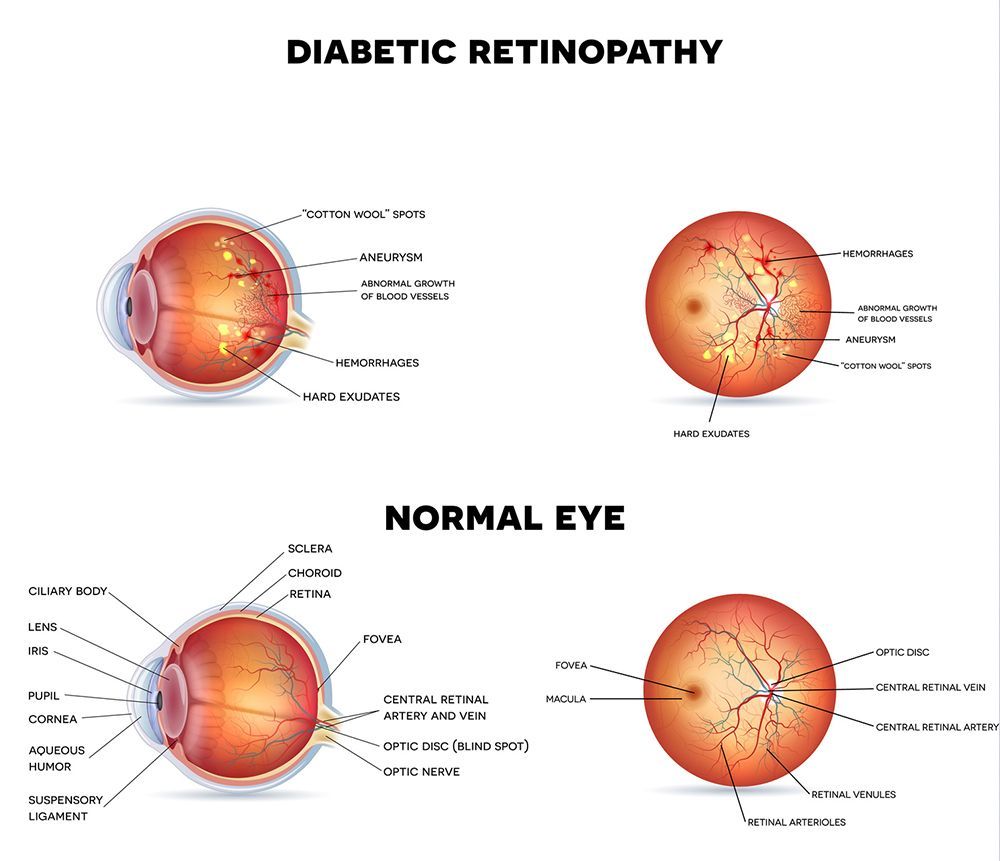
Diabetic Retinopathy
What is diabetic retinopathy?
Chronically high blood sugar from diabetes is associated with damage to the lining of the blood vessels in the retina, leading to
diabetic retinopathy. Diabetic retinopathy begins as an abnormality of the retinal blood vessels. Often, there are areas of the retina where circulation of blood is impaired or missing. Sometimes, as time goes on, fluid leaks from the retinal vessels causing swelling of the central retina and possibly vision loss. In its most advanced stage, new abnormal blood vessels grow on the surface of the retina, which can lead to bleeding and tractional detachment of the retina.
Who is at risk for diabetic retinopathy?
People with all types of diabetes (type 1, type 2, and gestational) are at risk for diabetic retinopathy. The risk of retinopathy due to diabetes increases the longer a person has diabetes, and with relatively poor blood sugar control. Patients with more severe grades of retinopathy are more prone to vision loss and need to be followed more closely. Patients with other medical problems, such as high blood pressure, high cholesterol, and kidney disease, are also more prone to vision loss from diabetic retinopathy. Women who develop or have diabetes during pregnancy may have rapid onset or worsening of diabetic retinopathy and need to be followed closely. Most diabetic patients need to be followed at least once a year by an eye doctor or retinal specialist. More frequent visits are often necessary.
What are the symptoms of diabetic retinopathy?
Sometimes, the vision can seem distorted or blurry if retinal or macular swelling develops due to diabetic retinopathy. It may be difficult to read, focus on road signs, and see fine details.
Sometimes, abnormal blood vessels may grow, which may bleed, causing spots to appear or a cloud to cover the vision. Sometimes, poor blood flow or traction on the retina may cause very poor vision.
Many times, diabetic retinopathy may progress silently. Screening examinations and appropriate follow up are very important since patients may not know that problems are developing in their eyes.
Are there any treatments for diabetic retinopathy?
Yes, there are a number of treatments that may be helpful in diabetic retinopathy.
Diabetic swelling can be treated with medications. Avastin, Lucentis, and Eylea are medications that are injected into the eye which can prevent blood vessels from leaking and bleeding in diabetic retinopathy. Patients with swelling due to diabetic retinopathy often have significant improvement in their vision if regular follow up and injections occur. Sometimes, steroid injections and sustained release steroid depots can be useful in treating diabetic macular edema, or swelling. Regular clinical examinations and OCT scans can determine when injections are needed. Fluorescein angiography can also be helpful at times.
Laser treatment can also help diabetic macular edema. Both standard and micropulse laser treatments can improve diabetic macular edema and give more durable treatment results than injection therapy. Laser treatments can be used in addition to injections and may result in patients needing fewer injections. Micropulse therapy may be applied more liberally than standard laser since it does not damage the retina.
When abnormal blood vessels grow on the surface of the retina, proliferative diabetic retinopathy (PDR) has occurred. PDR can be treated with laser therapy. Injections can also improve PDR. Sometimes, when bleeding or traction has occurred, vitrectomy surgery may be necessary to stabilize or improve vision.
In all cases, good blood sugar control is useful. Careful treatment of other medical conditions such as high blood pressure, high cholesterol, kidney disease, and obesity is also helpful to your eyes. We will keep your medical doctors informed of the status of your eyes. This information may be valuable to your diabetic doctor.
Although sometimes challenging, keeping regular follow up appointments is critical to maintaining vision in diabetic retinopathy.